Diagnosing and Treating Mast Cell Activation Syndrome (MCAS)
Mast cell activation syndrome (MCAS) is a complex and often misunderstood disorder of the immune system that occurs when mast cells — a type of white blood cell — trigger an excessive inflammatory response.
MCAS can cause a range of symptoms, including skin rashes, itching, flushing, bloating, constipation or diarrhea, difficulty breathing, fatigue, headaches, joint and muscle pain, and neurological symptoms. It often makes people hypersensitive to foods they never had a problem eating in the past.
Based on their symptoms, patients with MCAS are often diagnosed as having allergies, asthma, myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), postural tachycardia syndrome (POTS), an inflammatory bowel disease (such as Crohn’s or ulcerative colitis), or another medical condition. Meanwhile, their underlying MCAS, which is the root cause of their symptoms, remains undiagnosed and untreated.
If you’re experiencing the symptoms I described or you’ve been diagnosed as having one of the conditions I mentioned, you’ve probably been prescribed medication to alleviate your symptoms. Medication for symptom relief may be effective to some degree for a period of time, but it doesn’t fully address the underlying issue. As a result, you’re likely to continue to suffer.
Through this post, I’m hoping to increase awareness of mast cell activation syndrome, so more patients can get the right diagnosis and effective treatment.
Identifying Your Triggers
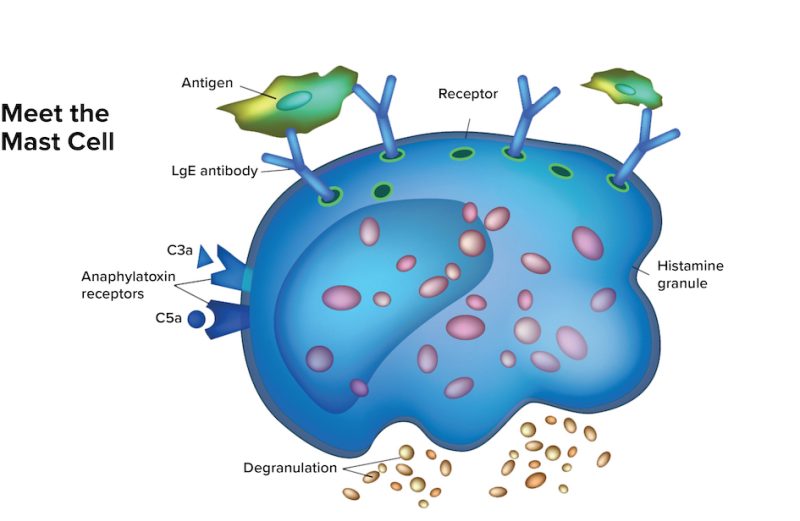
When they function properly, your mast cells play an important role in protecting your body against pathogens, such as infectious bacteria and viruses. When these cells perceive a potential threat, they release chemical mediators — including histamine — to launch a rapid immune response intended to destroy and eliminate the pathogen.
However, when these cells become overly sensitive, they release chemical mediators in response to non-threatening triggers. Sometimes, they release too much. Triggers vary among individuals and may include the following: Continue reading…